VN: Types and Diversity of Vegetarian Diets (2009)
To examine a variety of belief and demographic factors that are associated with the perception that meat is intrinsically unhealthful.
- Usable responses to mailed survey
- Vegetarians specifically recruited for the study.
None reported.
Recruitment
1,000 people in a southern Australian state were selected at random and questionnaires were mailed to them. Because of the low number of vegetarians in the number of respondents (N=9), a non-randomized sample of vegetarians was recruited via advertisements in health food stores, at vegetarian cafes and restaurants and at Adelaide University by distributing questionnaires at an environmental fair and by word-of-mouth.
Design
A 12-page booklet (200 items) was mailed to each person in the sample along with a cover letter and postage-paid envelope. Reminders were sent as follow-up.
Blinding Used
None.
Intervention
None.
Statistical Analysis
- Principal components analysis with varimax rotation was used to create factors
- Cross-tabulation analyses by sex and dietary group (non-vegetarian, semi-vegetarian, vegetarian) were done for each of the four items incorporated in the Meat is Unhealthy score
- Stepwise multiple regression was used to identify predictors of the belief that meat is unhealthful from the identified factors and demographic variables.
Timing of Measurements
Not reported.
Dependent Variables
Four specific questions (treated as a factor) designed to determine whether the subject believed that meat was unhealthful.
Independent Variables
- 20 items about beliefs about meat
- Perceived benefits of vegetarian diets (24 items)
- 13 demographic variables including age, sex, occupation, education, marital status, nature of household, income, religion and ethnicity
- Self-reported diet group (non-vegetarian, semi-vegetarian, vegetarian).
Initial N
- Survey mailed to 1,000 people selected at random: 603 answered the questionnaire; two surveys were unusable; 15% of the questionnaires were undeliverable. Only nine vegetarians were identified.
- Vegetarians and semi-vegetarians specifically recruited: 106.
Attrition (Final N)
Total number of usable questionnaires: 707.
Age
| Age (years) |
Non-Random Survey | Random Survey |
| 15-18 |
3.8
|
0.7
|
| 19-24 |
27.4
|
3.8
|
| 25-44 |
48.1
|
40.9
|
| 45-64 |
17
|
33.4
|
| 65+ |
3.8
|
21.2
|
Ethnicity
Not reported.
Other Relevant Demographics
| Employment Status | Non-Random Survey | Random Survey |
| Employed Full-Time |
17.9
|
29.8
|
| Employed Part-Time |
17.9
|
17.6
|
| Unemployed |
7.5
|
1.7
|
| Married |
38.5
|
69
|
| Divorced/Widowed |
10.6
|
17.4
|
Anthropometrics
Not reported.
Location
Australia.
The authors wanted to know what sorts of things are associated with the belief that meat is intrinsically unhealthful. They asked four questions designed to assess this belief.
Percentage Who Agree with the Specific Statement
| Specific Statement | Women | Men | |||||
| Non-Veg. | Semi-Veg. | Veg. | Non-Veg. | Semi-Veg. | Veg. | ||
| Meat causes heart disease. |
6
|
24
|
46
|
8
|
33
|
65
|
|
| Meat causes cancer. |
1
|
18
|
42
|
4
|
21
|
50
|
|
| Red meat is fattening. |
10
|
9
|
37
|
12
|
39
|
55
|
|
| Meat is unhealthy. |
2
|
12
|
56
|
4
|
33
|
73
|
|
- The authors first used a statistical procedure to identify survey items that were answered in similar ways (factors)
- They then ran another procedure to determine which of these factors helped predict the belief that meat is intrinsically unhealthy
- They found that the factors that explained the belief that meat is unhealthful varied by diet group.
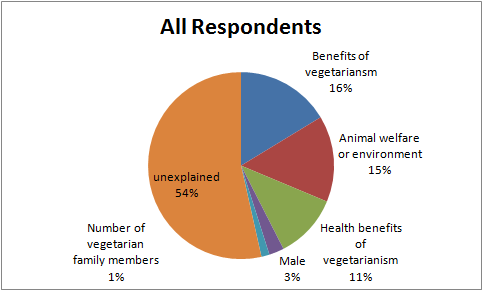
All Respondents
| All Respondents | Percentage Who Believe That Meat is Unhealthful Attitude Explained |
| Benefits of Vegetariansm |
16.3
|
| Animal Welfare or Environment |
15
|
| Health Benefits of Vegetarianism |
11.2
|
| Male |
2.6
|
| Number of Vegetarian Family Members |
1.4
|
| Unexplained |
53.5
|
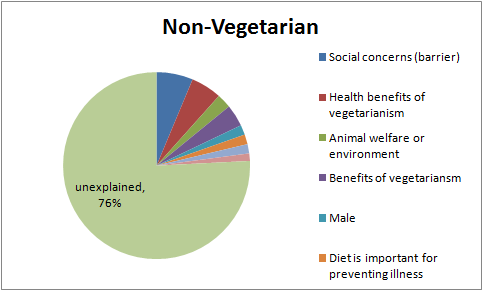
Non-Vegetarians
| Non-Vegetarian | Percentage Who Believe That Meat is Unhealthful Attitude Explained |
| Social Concerns (Barrier) |
6.3
|
| Health Benefits of Vegetarianism |
5.3
|
| Animal Welfare or Environment |
2.5
|
| Benefits of Vegetarianism |
3.8
|
| Male |
1.7
|
| Diet is Important for Preventing Illness |
1.7
|
| Recall of Meat Promotion |
1.6
|
| Recall of Vegetarian Promotion |
1.3
|
| Unexplained |
75.8
|
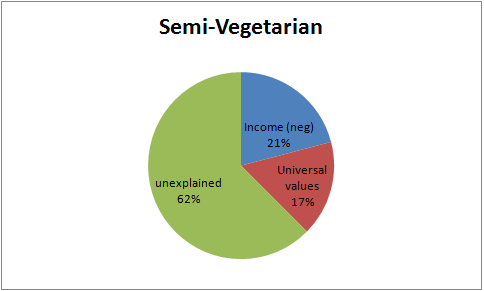
Semi-Vegetarians
| Semi-Vegetarianism | Percentage Who Believe That Meat is Unhealthful Attitude Explained |
| Income (Neg) |
20.9
|
| Universal Values |
16.6
|
| Unexplained |
62.5
|
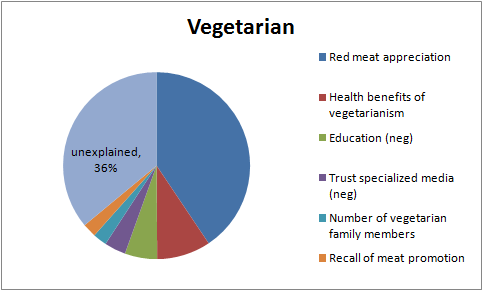
Vegetarians
| Vegetarian | Percentage Who Believe That Meat is Unhealthful Attitude Explained |
| Red Meat Appreciation |
40.6
|
| Health Benefits of Vegetarianism |
9.3
|
| Education (Neg) |
5.6
|
| Trust Specialized Media (Neg) |
3.7
|
| Number of Vegetarian Family Members |
2.4
|
| Recall of Meat Promotion |
2.4
|
| Unexplained |
36
|
Observations
- Overall, the perceived benefits of vegetarianism were the strongest predictor of the belief that meat is unhealthful. Peace and contentment benefits of vegetarianism was the key factor. However, this factor was diverse, including such items as equality between sexes, reduced aggression and religious and spiritual benefits.
- The results also show a strong association between the concern for animal welfare, food-production efficiency with the environment and beliefs about the unhealthfullness of meat
- The perceived health benefits of vegetarianism also predicted beliefs that meat is unhealthful
- Social issues were also important among non-vegetarians: The fact that barriers to vegetarianism were positively associated with the belief that meat is unhealthful could show a need to justify meat-eating behaviors among non-vegetarians
- Red meat appreciation positively predicted the belief that meat is unhealthful. At first, this seems to be an odd finding, however it indicates that as vegetarians become less strongly negative about meat appreciation, the more they agree that meat is intrinsically unhealthful. This may be because people who appreciate red meat may need a different reason to not eat meat (i.e., the belief that it is unhealthful).
- Income and education were the only demographic variables associated with the belief that meat is unhealthful and both were negative predictors. That is, as education increased, the belief that meat is intrinsically unhealthful decreased (which may be expected as the better educated they are, the less likely they are to believe that meat causes illness). Likewise, as income increased, the belief that meat was unhealthful decreased. More highly-educated and wealthy vegetarians may simply have other reasons to be vegetarian than the belief that meat is unhealthful.
Policy Implications
More education is needed to overcome misconceptions about the healthfulness of meat; for instance, that meat does not cause illness (although meat consumption is associated with some diseases).
- We found that negative beliefs about the health aspects of meat were linked predominantly to the perceived benefits of vegetarianism for all respondents considered as a group and, to a lesser extent, for non-vegetarians and vegetarians
- Social concerns about vegetarianism and health benefits were most important for non-vegetarians, whereas red meat appreciation and health benefits of vegetarianism were important for vegetarians
- To influence meat consumption via beliefs about the healthfulness of meat, it is important to address social, environmental, animal welfare, peace and contentment issues as well as health.
| University/Hospital: | Adelaide University, Deakin University |
- Well-designed study
- Cross-sectional design limits the ability to determine the direction of influences
- Random sample was supplemented by a non-randomized recruitment of vegetarians and semi-vegetarians.
|
Quality Criteria Checklist: Primary Research
|
|||
| Relevance Questions | |||
| 1. | Would implementing the studied intervention or procedure (if found successful) result in improved outcomes for the patients/clients/population group? (Not Applicable for some epidemiological studies) | N/A | |
| 1. | Would implementing the studied intervention or procedure (if found successful) result in improved outcomes for the patients/clients/population group? (Not Applicable for some epidemiological studies) | N/A | |
| 2. | Did the authors study an outcome (dependent variable) or topic that the patients/clients/population group would care about? | Yes | |
| 2. | Did the authors study an outcome (dependent variable) or topic that the patients/clients/population group would care about? | Yes | |
| 3. | Is the focus of the intervention or procedure (independent variable) or topic of study a common issue of concern to dieteticspractice? | Yes | |
| 3. | Is the focus of the intervention or procedure (independent variable) or topic of study a common issue of concern to dieteticspractice? | Yes | |
| 4. | Is the intervention or procedure feasible? (NA for some epidemiological studies) | N/A | |
| 4. | Is the intervention or procedure feasible? (NA for some epidemiological studies) | N/A | |
| Validity Questions | |||
| 1. | Was the research question clearly stated? | Yes | |
| 1. | Was the research question clearly stated? | Yes | |
| 1.1. | Was (were) the specific intervention(s) or procedure(s) [independent variable(s)] identified? | Yes | |
| 1.1. | Was (were) the specific intervention(s) or procedure(s) [independent variable(s)] identified? | Yes | |
| 1.2. | Was (were) the outcome(s) [dependent variable(s)] clearly indicated? | Yes | |
| 1.2. | Was (were) the outcome(s) [dependent variable(s)] clearly indicated? | Yes | |
| 1.3. | Were the target population and setting specified? | Yes | |
| 1.3. | Were the target population and setting specified? | Yes | |
| 2. | Was the selection of study subjects/patients free from bias? | Yes | |
| 2. | Was the selection of study subjects/patients free from bias? | Yes | |
| 2.1. | Were inclusion/exclusion criteria specified (e.g., risk, point in disease progression, diagnostic or prognosis criteria), and with sufficient detail and without omitting criteria critical to the study? | Yes | |
| 2.1. | Were inclusion/exclusion criteria specified (e.g., risk, point in disease progression, diagnostic or prognosis criteria), and with sufficient detail and without omitting criteria critical to the study? | Yes | |
| 2.2. | Were criteria applied equally to all study groups? | No | |
| 2.2. | Were criteria applied equally to all study groups? | No | |
| 2.3. | Were health, demographics, and other characteristics of subjects described? | Yes | |
| 2.3. | Were health, demographics, and other characteristics of subjects described? | Yes | |
| 2.4. | Were the subjects/patients a representative sample of the relevant population? | Yes | |
| 2.4. | Were the subjects/patients a representative sample of the relevant population? | Yes | |
| 3. | Were study groups comparable? | Yes | |
| 3. | Were study groups comparable? | Yes | |
| 3.1. | Was the method of assigning subjects/patients to groups described and unbiased? (Method of randomization identified if RCT) | No | |
| 3.1. | Was the method of assigning subjects/patients to groups described and unbiased? (Method of randomization identified if RCT) | No | |
| 3.2. | Were distribution of disease status, prognostic factors, and other factors (e.g., demographics) similar across study groups at baseline? | Yes | |
| 3.2. | Were distribution of disease status, prognostic factors, and other factors (e.g., demographics) similar across study groups at baseline? | Yes | |
| 3.3. | Were concurrent controls or comparisons used? (Concurrent preferred over historical control or comparison groups.) | Yes | |
| 3.3. | Were concurrent controls or comparisons used? (Concurrent preferred over historical control or comparison groups.) | Yes | |
| 3.4. | If cohort study or cross-sectional study, were groups comparable on important confounding factors and/or were preexisting differences accounted for by using appropriate adjustments in statistical analysis? | Yes | |
| 3.4. | If cohort study or cross-sectional study, were groups comparable on important confounding factors and/or were preexisting differences accounted for by using appropriate adjustments in statistical analysis? | Yes | |
| 3.5. | If case control study, were potential confounding factors comparable for cases and controls? (If case series or trial with subjects serving as own control, this criterion is not applicable.) | Yes | |
| 3.5. | If case control study, were potential confounding factors comparable for cases and controls? (If case series or trial with subjects serving as own control, this criterion is not applicable.) | Yes | |
| 3.6. | If diagnostic test, was there an independent blind comparison with an appropriate reference standard (e.g., "gold standard")? | N/A | |
| 3.6. | If diagnostic test, was there an independent blind comparison with an appropriate reference standard (e.g., "gold standard")? | N/A | |
| 4. | Was method of handling withdrawals described? | Yes | |
| 4. | Was method of handling withdrawals described? | Yes | |
| 4.1. | Were follow-up methods described and the same for all groups? | N/A | |
| 4.1. | Were follow-up methods described and the same for all groups? | N/A | |
| 4.2. | Was the number, characteristics of withdrawals (i.e., dropouts, lost to follow up, attrition rate) and/or response rate (cross-sectional studies) described for each group? (Follow up goal for a strong study is 80%.) | Yes | |
| 4.2. | Was the number, characteristics of withdrawals (i.e., dropouts, lost to follow up, attrition rate) and/or response rate (cross-sectional studies) described for each group? (Follow up goal for a strong study is 80%.) | Yes | |
| 4.3. | Were all enrolled subjects/patients (in the original sample) accounted for? | N/A | |
| 4.3. | Were all enrolled subjects/patients (in the original sample) accounted for? | N/A | |
| 4.4. | Were reasons for withdrawals similar across groups? | N/A | |
| 4.4. | Were reasons for withdrawals similar across groups? | N/A | |
| 4.5. | If diagnostic test, was decision to perform reference test not dependent on results of test under study? | N/A | |
| 4.5. | If diagnostic test, was decision to perform reference test not dependent on results of test under study? | N/A | |
| 5. | Was blinding used to prevent introduction of bias? | Yes | |
| 5. | Was blinding used to prevent introduction of bias? | Yes | |
| 5.1. | In intervention study, were subjects, clinicians/practitioners, and investigators blinded to treatment group, as appropriate? | N/A | |
| 5.1. | In intervention study, were subjects, clinicians/practitioners, and investigators blinded to treatment group, as appropriate? | N/A | |
| 5.2. | Were data collectors blinded for outcomes assessment? (If outcome is measured using an objective test, such as a lab value, this criterion is assumed to be met.) | Yes | |
| 5.2. | Were data collectors blinded for outcomes assessment? (If outcome is measured using an objective test, such as a lab value, this criterion is assumed to be met.) | Yes | |
| 5.3. | In cohort study or cross-sectional study, were measurements of outcomes and risk factors blinded? | Yes | |
| 5.3. | In cohort study or cross-sectional study, were measurements of outcomes and risk factors blinded? | Yes | |
| 5.4. | In case control study, was case definition explicit and case ascertainment not influenced by exposure status? | N/A | |
| 5.4. | In case control study, was case definition explicit and case ascertainment not influenced by exposure status? | N/A | |
| 5.5. | In diagnostic study, were test results blinded to patient history and other test results? | N/A | |
| 5.5. | In diagnostic study, were test results blinded to patient history and other test results? | N/A | |
| 6. | Were intervention/therapeutic regimens/exposure factor or procedure and any comparison(s) described in detail? Were interveningfactors described? | Yes | |
| 6. | Were intervention/therapeutic regimens/exposure factor or procedure and any comparison(s) described in detail? Were interveningfactors described? | Yes | |
| 6.1. | In RCT or other intervention trial, were protocols described for all regimens studied? | N/A | |
| 6.1. | In RCT or other intervention trial, were protocols described for all regimens studied? | N/A | |
| 6.2. | In observational study, were interventions, study settings, and clinicians/provider described? | Yes | |
| 6.2. | In observational study, were interventions, study settings, and clinicians/provider described? | Yes | |
| 6.3. | Was the intensity and duration of the intervention or exposure factor sufficient to produce a meaningful effect? | N/A | |
| 6.3. | Was the intensity and duration of the intervention or exposure factor sufficient to produce a meaningful effect? | N/A | |
| 6.4. | Was the amount of exposure and, if relevant, subject/patient compliance measured? | N/A | |
| 6.4. | Was the amount of exposure and, if relevant, subject/patient compliance measured? | N/A | |
| 6.5. | Were co-interventions (e.g., ancillary treatments, other therapies) described? | N/A | |
| 6.5. | Were co-interventions (e.g., ancillary treatments, other therapies) described? | N/A | |
| 6.6. | Were extra or unplanned treatments described? | N/A | |
| 6.6. | Were extra or unplanned treatments described? | N/A | |
| 6.7. | Was the information for 6.4, 6.5, and 6.6 assessed the same way for all groups? | N/A | |
| 6.7. | Was the information for 6.4, 6.5, and 6.6 assessed the same way for all groups? | N/A | |
| 6.8. | In diagnostic study, were details of test administration and replication sufficient? | N/A | |
| 6.8. | In diagnostic study, were details of test administration and replication sufficient? | N/A | |
| 7. | Were outcomes clearly defined and the measurements valid and reliable? | Yes | |
| 7. | Were outcomes clearly defined and the measurements valid and reliable? | Yes | |
| 7.1. | Were primary and secondary endpoints described and relevant to the question? | Yes | |
| 7.1. | Were primary and secondary endpoints described and relevant to the question? | Yes | |
| 7.2. | Were nutrition measures appropriate to question and outcomes of concern? | Yes | |
| 7.2. | Were nutrition measures appropriate to question and outcomes of concern? | Yes | |
| 7.3. | Was the period of follow-up long enough for important outcome(s) to occur? | N/A | |
| 7.3. | Was the period of follow-up long enough for important outcome(s) to occur? | N/A | |
| 7.4. | Were the observations and measurements based on standard, valid, and reliable data collection instruments/tests/procedures? | Yes | |
| 7.4. | Were the observations and measurements based on standard, valid, and reliable data collection instruments/tests/procedures? | Yes | |
| 7.5. | Was the measurement of effect at an appropriate level of precision? | Yes | |
| 7.5. | Was the measurement of effect at an appropriate level of precision? | Yes | |
| 7.6. | Were other factors accounted for (measured) that could affect outcomes? | Yes | |
| 7.6. | Were other factors accounted for (measured) that could affect outcomes? | Yes | |
| 7.7. | Were the measurements conducted consistently across groups? | Yes | |
| 7.7. | Were the measurements conducted consistently across groups? | Yes | |
| 8. | Was the statistical analysis appropriate for the study design and type of outcome indicators? | Yes | |
| 8. | Was the statistical analysis appropriate for the study design and type of outcome indicators? | Yes | |
| 8.1. | Were statistical analyses adequately described and the results reported appropriately? | Yes | |
| 8.1. | Were statistical analyses adequately described and the results reported appropriately? | Yes | |
| 8.2. | Were correct statistical tests used and assumptions of test not violated? | Yes | |
| 8.2. | Were correct statistical tests used and assumptions of test not violated? | Yes | |
| 8.3. | Were statistics reported with levels of significance and/or confidence intervals? | Yes | |
| 8.3. | Were statistics reported with levels of significance and/or confidence intervals? | Yes | |
| 8.4. | Was "intent to treat" analysis of outcomes done (and as appropriate, was there an analysis of outcomes for those maximally exposed or a dose-response analysis)? | N/A | |
| 8.4. | Was "intent to treat" analysis of outcomes done (and as appropriate, was there an analysis of outcomes for those maximally exposed or a dose-response analysis)? | N/A | |
| 8.5. | Were adequate adjustments made for effects of confounding factors that might have affected the outcomes (e.g., multivariate analyses)? | Yes | |
| 8.5. | Were adequate adjustments made for effects of confounding factors that might have affected the outcomes (e.g., multivariate analyses)? | Yes | |
| 8.6. | Was clinical significance as well as statistical significance reported? | Yes | |
| 8.6. | Was clinical significance as well as statistical significance reported? | Yes | |
| 8.7. | If negative findings, was a power calculation reported to address type 2 error? | N/A | |
| 8.7. | If negative findings, was a power calculation reported to address type 2 error? | N/A | |
| 9. | Are conclusions supported by results with biases and limitations taken into consideration? | Yes | |
| 9. | Are conclusions supported by results with biases and limitations taken into consideration? | Yes | |
| 9.1. | Is there a discussion of findings? | Yes | |
| 9.1. | Is there a discussion of findings? | Yes | |
| 9.2. | Are biases and study limitations identified and discussed? | Yes | |
| 9.2. | Are biases and study limitations identified and discussed? | Yes | |
| 10. | Is bias due to study's funding or sponsorship unlikely? | Yes | |
| 10. | Is bias due to study's funding or sponsorship unlikely? | Yes | |
| 10.1. | Were sources of funding and investigators' affiliations described? | No | |
| 10.1. | Were sources of funding and investigators' affiliations described? | No | |
| 10.2. | Was the study free from apparent conflict of interest? | Yes | |
| 10.2. | Was the study free from apparent conflict of interest? | Yes | |